-

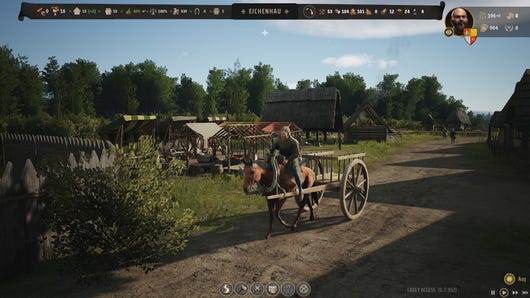
Review: Another Crab's Treasure review: a playful Soulslike for everyone, especially if you like crabs
This will more than tide you over
-

Review: Sand Land review: a boring Mad Max lite that should have been very exciting
More like Bland Land, am I right?
-

Latest Horizon Forbidden West PC patch finally fixes its weirdest issue
Nvidia Reflex, you’ve bested me for the last time
-

The original Fallout is the perfect antidote to Fallout fever
War did change, actually
-

The kissable frogs and sparky combat of Hades 2 looks set to bewitch fans
Impressions of the "technical test"
-

Whatever the Fallout TV show does with New Vegas lore, Josh Sawyer doesn’t care: “It was never mine”
The Obsidian design director on Pillars of Eternity II burnout and living with dead projects
-
Lethal Company gets worse as you get better
Why being dumb is good, actually
-
The Maw - 22nd-27th April 2024
This week's least outwardly offputting game releases, plus our weekly newsblog
Live -
Should You Bother With... Hall effect keyboards?
Heroes of might and magnets
Psst! Explore our new "For you" section and get personalised recommendations about what to read.
-

£25 for a pair of speakers sounds great to us
These Creative Pebble V3 speakers are a great choice for rich, clear audio on a budget.
-

Get the fastest PCIe 4.0 SSD for $139 at Amazon
Save over $50 on the Crucial T500.
-

You can get a WD Black SN850X 2TB SSD for as little as £112 but they're selling fast
Save up to £28 on this speedy SSD using the eBay app and a special discount code.
-

The Crucial P3 2TB, one of the fastest 3.0 SSDs, is on sale for just £85
Get a big chunk of storage space for a bargain price.
-

Erangel Classic returns for two weeks next month
-
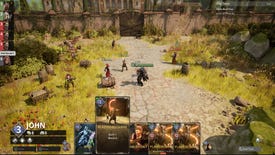
Former Fable devs reveal a new co-op RPG, then announce its development is on hold amid layoffs
Flaming Fowl will shift to a smaller game they can fund themselves
-

The ‘Agent Trevor’ pack would’ve accompanied zombie and alien-themed expansions
-

Head of Ori and the Blind Forest studio says there’s “just no way” they could’ve shipped the game without player feedback
-

Minecraft rolls out armadillo mob and rewilds biomes with eight new wolf variants
Chewier on the inside
-

Lords Of The Fallen's latest update adds cruel modifiers that turn it into a roguelike
One for the masochists
-
The Don't Starve devs' new cutesy co-cop dungeon crawler is out in early access today
Rotwood allows you and up to three friends to kill a tree
-
You can now pre-register for Genshin developer's Zenless Zone Zero
It's due sometime in the first half of 2024
-

Supporters only: Watching Civil War made me want more games with black and white stances on morality
I can't think of any good modern examples!
I went to see Civil War this weekend. I liked a bunch of it, didn't like a bunch of it. One thing I thought was very obvious is that it sanitises its titular conflict of any political context. On the one hand, I understand this as part of the theming, said almost directly into the camera by Kirsten Dunst's photojournalist character: as journalists they're there …
-

Supporters only: Piecing It Together gave me a timely little island of calm
Good thing I got my pieces
-
Supporters only: What are ‘solvable’ games, and is being solvable a bad thing?
Balatroptimisation
-
Supporters only: An action platformer about getting an eye back from ants affirms my belief that games need a Ronseal approach to their titles
Ants Took My Eyeball is about a man who has had his eyeball taken. By ants.
Get your first month for £1 (normally £3.99) when you buy a Standard Rock Paper Shotgun subscription. Enjoy ad-free browsing, our monthly letter from the editor, and discounts on RPS merch. Your support helps us create more great writing about PC games.
See more information-

Review: Another Crab's Treasure review: a playful Soulslike for everyone, especially if you like crabs
This will more than tide you over
-

Review: Sand Land review: a boring Mad Max lite that should have been very exciting
More like Bland Land, am I right?
-

Review: Tales Of Kenzera: Zau review: a beautifully designed yet imprecise platforming adventure
It's not time to make a change
-

The best farming games like Stardew Valley on PC
The cream of the crop
-

A very puzzling collection
-

The 15 best open world games on PC
Keep your options open
-

Review: Botany Manor review: peaceful and beautiful best-in-show plant puzzles
Come away, O human child! To the waters and the wild
-

Should You Bother With... Hall effect keyboards?
Heroes of might and magnets
-

Arise now, ye Cerim: No Rest for the Wicked’s performance updates are underway
Already running better on low-end GPUs
-

No Rest for the Wicked’s PC performance suggests the wicked might be better off waiting
Got them early access growing pains
-

After six months of renovations, Cities: Skylines 2 performance is considerably less terrible
Some GPUs get more than double the frames since launch
-

Innkeep satisfies my craving for a fantasy game that's just a grim drudgery simulator
Something need doing?
-

Hellish indie horror IRIS can get in the toaster and I’m sure the feeling is mutual
Actively hostile to my attempts to not put it straight in the toaster
-
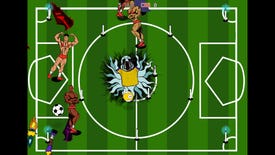
Cereballers is a free 2D football parody with a spark of real genius
The offside rule is the least of your problems
-

Erangel Classic returns for two weeks next month
-

Former Fable devs reveal a new co-op RPG, then announce its development is on hold amid layoffs
Flaming Fowl will shift to a smaller game they can fund themselves
-

The ‘Agent Trevor’ pack would’ve accompanied zombie and alien-themed expansions
-

Head of Ori and the Blind Forest studio says there’s “just no way” they could’ve shipped the game without player feedback
-

Should You Bother With... Hall effect keyboards?
Heroes of might and magnets
-

Review: Another Crab's Treasure review: a playful Soulslike for everyone, especially if you like crabs
This will more than tide you over
-
Review: Sand Land review: a boring Mad Max lite that should have been very exciting
More like Bland Land, am I right?
-
Supporters only: Watching Civil War made me want more games with black and white stances on morality
I can't think of any good modern examples!
-
Minecraft rolls out armadillo mob and rewilds biomes with eight new wolf variants
Chewier on the inside
-

Here's an archive of previous Wordle words
-
Today's NYT Connections hint and answers (Thu, Apr 25)
Need a hint for today's Connections? Read our guide for help with Connections #319
-

Wordle hint and answer today #1041 (April 25 2024)
Stuck on today's Wordle word for April 25? Read our hint or find the answer below!
-

Genshin Impact codes [April 2024]
All the currently active Genshin Impact codes on offer
-

Fallout 4: Best Power Armor and where to find
Here are the best Power Armor sets in Fallout 4 and where to find them
-

NYT Connections hint and answers (Wed, Apr 24)
Need a hint for Connections? Read our guide for help with Connections #318
-
Wordle hint and answer #1040 (April 24 2024)
Stuck on today's the word for April 24? Read our hint or find the answer below!
-
NYT Connections hint and answers (Tue, Apr 23)
Need a hint for today's Connections? Read our guide for help with Connections #317
-
Wordle hint and answer #1039 (April 23 2024)
Stuck on today's Wordle word for April 23? Read our hint or find the answer below!
-
Whether cop or robber, you'll benefit from the freebies these codes get you